What is Virtual Care?
Telehealth has never been more important than in the COVID-19 pandemic. At the centre of any successful telehealth strategy must be Virtual Care, this article will define what it is, why it is important, what the key challenges are, and how it can improve in future.
What is Virtual Care?
There are a few different definitions of Virtual Care. At STL Partners we see Virtual Care as being any service that leverages phone / video conferencing / online tools to replace scheduled appointments with healthcare professionals, either GPs or specialised. Virtual Care is just one component of telehealth overall, for example we do not include remote patient monitoring (collecting electronic health data or questionnaires from patients not in a healthcare facility to track patient status).
Virtual Care does not just include patient-to-healthcare provider interaction, but also provider-to-provider interaction. This may include discussing patient diagnoses or reviewing pharmacy prescriptions. Provider-to-provider transfer of health records or patient information is included as well.
Figure 1: Different types of digital health services

Why demand for Virtual Care is increasing
As COVID-19 has restricted face-to-face meetings, there has been an exponential increase in the need for Virtual Care services. However, it can create great value outside of a pandemic world as well. Patients are able to more easily interact with medical specialists who may be located far away, or perhaps if they just want to seek a second opinion. It is also valuable for patients who may be movement impaired or simply are located far away from the nearest GP.
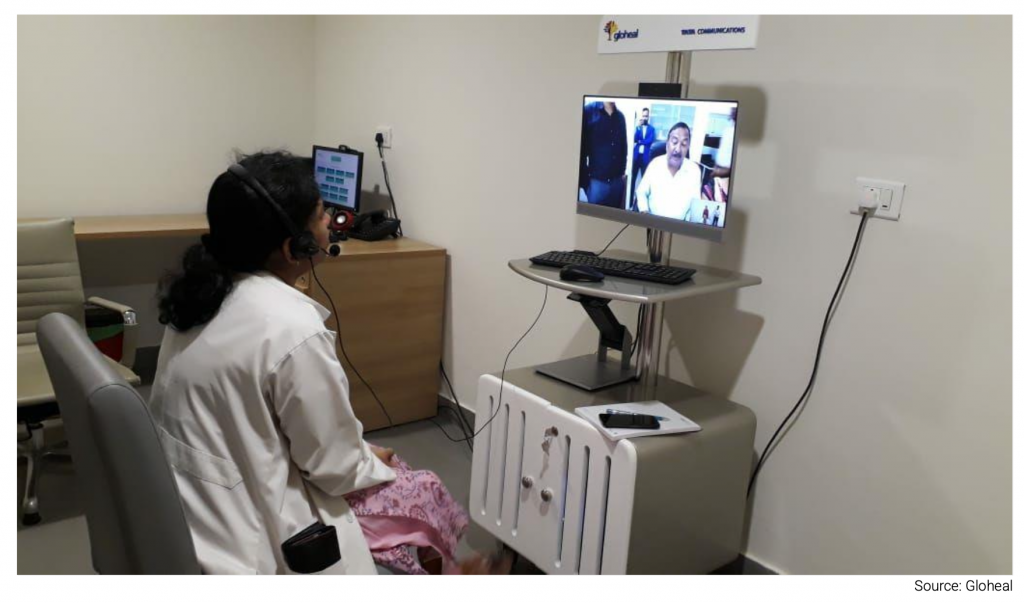
This can be particularly useful in developing countries where rural communities may be located long distances from healthcare professionals or are unable to travel to a healthcare facility. Tata Communications have launched a virtual clinic service called Gloheal to try and service these communities. People can go to specific stations and communicate with healthcare specialists. Tata provides the whole solution, including IT, connectivity, platform, and the app to the healthcare organisation. There are clear opportunities for telcos in other countries to take on similar business models to service rural communities.
Figure 2: Gloheal’s virtual clinic service provided by Tata Group
Virtual Care ranges from basic virtual consultations to increasingly more advanced services. Advanced digital tools such as natural language processing to help doctors save time taking notes will bring great value to solutions. AI should unlock lots of new features and Virtual Care services will only continue to become more comprehensive.
Challenges for Virtual Care
The suitability of Virtual Care for different types of consultations or healthcare professionals will clearly vary. COVID-19 has gone some way to demonstrating what type of consultations are more or less suited to Virtual Care. Regulatory barriers have been brought down, but tangible proof points have also been provided to patients and physicians.
Patient experience
It has been said that purely virtual interactions with patients will create too impersonal of a patient experience, however there is little evidence that in-person patient experiences were particularly personal before COVID-19. A study published in the Journal of General Internal Medicine found that 64% of primary care providers and 80% of specialists did not bother asking patients why they came in and they interrupted the patient after a median of 11 seconds. That being said, the need for an in-person patient experience will likely depend on the type of consultation. For example, consultants in psychosexual medicine need to create real emotional and physical connections with patients, whereas many GP consultations can be carried out effectively over the phone. Virtual care will suit certain consultations better than others.
Quality of care
Another concern that is raised is around quality of care, indeed in a survey by Beckers Hospital Review 10% of patients listed this as a concern. There is little evidence to support that this would be the case, and in fact by improving access to care through lower costs and fewer barriers to healthcare provision, Virtual Care will likely increase quality of care. STL Partners estimates that by 2030 rising digital health penetration will save countries roughly $645bn globally (this is an extra $297bn due to the impact of COVID-19). However, as with the need for in-person consultations for patient experience, the suitability of Virtual Care will depend on the type of consultation.
Whilst many issues can be diagnosed using Virtual Care, there are clearly many diagnoses which are not so easy to make. The advantage of Virtual Care however, is that the clinician will be able to schedule an in-person appointment in real-time and will already have an idea of the symptoms and general patient condition which will make the in-person appointment more efficient.
Clinician burnout
Clinician burnout is one way that quality of care may be affected according to some critics, healthcare professionals may be on back-to-back virtual consultations without the natural break between patients that is afforded in face-to-face settings. Now that they are able to work from everywhere there is not the separation usually afforded by the hospital and longer hours may result. However, it is also possible that the opposite is true, able to work from home practitioners will be free of the hassle attached to travel to healthcare facilities or, even more draining, travel to the home of patients. This is more likely to reduce clinician burnout than to increase it. The impact will likely depend on the individual healthcare professional.
Data security
Data security is an area of concern for some people. Instead of sharing personal information face-to-face patients are sharing it over audio or video link, this is potentially less secure. Steps can be taken to reduce this risk including two-factor authentication and encrypted data transmission.
Some of the challenges with Virtual Care can be at least partly resolved by new and developing technologies. Virtual Care in its current form certainly causes understandable concern or doubt amongst some patients. However, as Virtual Care improves this should lessen, and much of this improvement should come through new technologies.
The role of 5G, edge computing and AI
The advent of 5G is cause for great optimism in digital health circles. It should significantly improve the application of Virtual Care. Greater bandwidth and lower latency will allow for much higher quality video streaming. This will be particularly useful for improving how many diagnoses can be made remotely as healthcare practitioners will be able to see higher quality images. It should also improve the overall experience as patients will be less likely to be subjected to distorted audio or video when trying to speak to practitioners. 5G is also more secure than previous mobile technologies so there should be less concern around data security.
That being said, one of the main applications of Virtual Care is to reach remote communities who are located very far from the nearest healthcare practitioner. Whilst they are likely to have 5G coverage in the future, it will be a long time before this happens. Moreover, often Virtual Care is useful for accessing patients who are less mobile, they tend to be elderly and on average have a lower grasp of new technologies. As a result, 5G may not have a large impact on the delivery of some aspects of Virtual Care for a while, but no doubt it can benefit many groups in the short term and these groups will only grow as time passes.
Edge computing is another area that can help with the delivery of Virtual Care. For calls that are at least relatively local to each other (i.e. same city or region) the lower latency can further reduce any distortion to audio or video. It can also ensure health data sent from the patient to the practitioner (e.g. live data from a heart-rate reading) is more real-time, thanks to the lower latency.
Where edge can be particularly useful in digital health in general is with data security. In-person health appointments usually allow health data to be kept in local servers, this is of course complicated when consultations are done from remote locations as in Virtual Care. Edge servers located at mobile stations would allow sensitive health data to be kept local to the stations as opposed to being sent via the cloud to be held elsewhere.
As highlighted previously, AI is another technology which should unlock a lot of new value through Virtual Care. AI technology can help with diagnosis via video link, analysing the feed to pick up signs the practitioner may have missed. AI with access to big data will be able to detect cases with similar symptoms and give diagnoses based on the whole database, as opposed to just the personal experience of the practitioner. Technology that can take notes for doctors (as previously mentioned) will also bring great value in allowing practitioners to concentrate fully on the patient, not only will this improve outcomes, but it also will help to maintain the patient-provider personal connection.
Virtual Care stands to benefit greatly from new technology. As we have seen in the COVID-19 pandemic, it has an increasing role to play in the future of healthcare and new technology such as 5G, edge computing, and AI will only accelerate its ability to cater to more people in an effective way. There are reasonable challenges to its current ability to deal with all cases, but these challenges can be minimised as new technology spreads into new markets. Virtual Care has the potential to permanently change our ability to provision healthcare for those most in need, and it is through the adoption of new technology that this will be achieved.
Implications for telcos
Some operators have recently launched or accelerated their deployment of virtual care services in response to COVID-19, these include Hong Kong Telecom, Globe Telecom and NOS. Virtual Care could provide a good anchor use case for entry into the digital health market for telcos: it is increasing in prevalence due to the pandemic and there is a lower barrier to entry compared with data transformation. Virtual Care therefore, may provide telcos with the tactical opportunity to build a health foundation on top of which they will be able to scale their healthcare businesses.
Author: Matt Bamforth is a Consultant at STL Partners specialising in 5G, Edge computing and private networks topics
Digital health insights pack
This 24-page document will provide you with a summary of insights from our healthcare research and consulting work:
- Key trends in the healthcare industry
- The role for telecoms: applications and business models
- Strategies for success: where to start
- How STL Partners can support you
Request the free digital health insights pack by clicking on button below:
![]()
Get in touch with our Digital Health Leads

Read more about digital health
Webinar
Telcos in health webinar
In this session Amy Cameron and Yesmean Luk looked at the opportunities for telcos in health. As a growing industry, with a national focus and significant digitisation challenges, healthcare is an attractive vertical for telcos seeking to build new revenues beyond core communications services.
Research
TELUS Health: Innovation leader case study
Healthcare is an attractive vertical for telcos to address with digital solutions. Although many telcos have made attempts to capture this opportunity, TELUS stands out as an example of the value of a long-term commitment to healthcare. In this case study, we examine TELUS’ strategy in health, evidence of its success, and draw out lessons for other telcos